Before the COVID-19 pandemic, we were dealing with the opioid 'crisis,' which continues to plague us.
I haven’t talked about this topic before, but the opioid crisis has affected my family very deeply and on many levels. It has touched us physically and emotionally in ways you never hear mentioned in the news. I understand that opioid addiction is a real problem. However, the war waged on opioids by the government and the medical community is preventing people who genuinely need effective pain medication from getting the treatment they need to live a life that’s remotely tolerable, let alone satisfying and happy.
Hitting Home
My dad has been permanently disabled for 27 years. He is an Army veteran who suffers from a painful spine injury caused when his back slammed into the hard steel interior of the tank he was inside as it rolled down a hill in Germany in 1975. That injury, combined with the additional spine issues he developed during his work as a dock worker (and an experimental surgery that followed), all left him with chronic, debilitating pain.
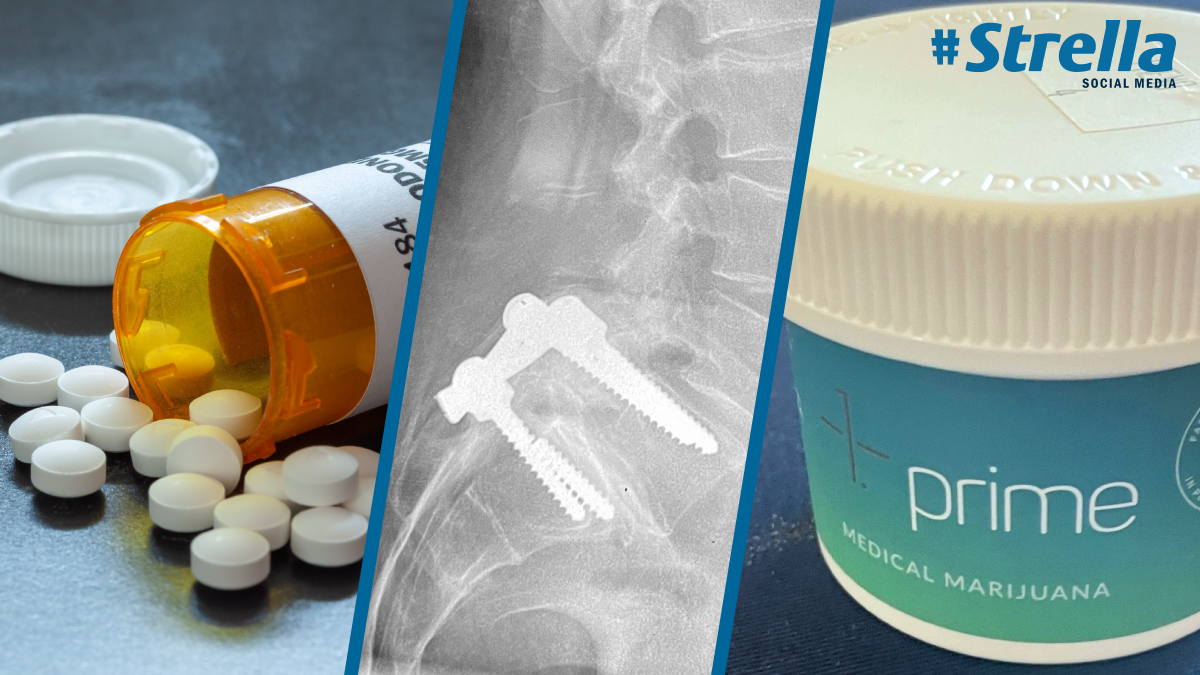
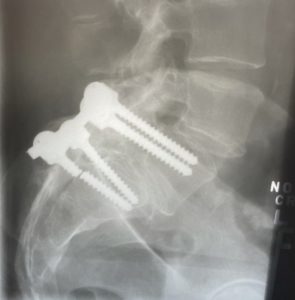
My father is in constant agony. Several surgical plates and screws have come loose in his back, and the screws are pressing on the nerves affecting his legs. His journey has brought him to several pain management doctors and the VA hospital, the latter of which provided the worst experience of all—but that’s a story for another day. He has tried many treatments—injections, water therapy, Aleve (way too much Aleve!)—but nothing is giving him relief. He even got approved for a medical marijuana (MMJ) card, but the weed makes him zone out and essentially want to do nothing at all.
Last week, Dad told me that he just wants a chance to have one good day before he dies. He hasn’t had a single good day in over two years. It breaks my heart. He’s only 64 years old and is giving up.
No one should have to live like that. And I am fighting for my father, who legitimately needs pain medication to have any measure of what most of us would consider “quality of life.” However, physicians refuse to prescribe him the only medicine that gives him relief.
Perspective From a Recovered Addict (My Brother)
My father is not an opioid addict. I say that because I feel qualified to know the difference as my brother is a recovered alcoholic and drug addict. Fortunately, Matt has been 16 months sober and on a healthier, happier path than before. I asked him what the difference is between an addict and someone who truly needs some form of medication to have any quality of life.
Matt told me, “An addict is someone who is leaning on a drug for selfish needs. It’s a psychological, not physical need, for them to numb themselves from the outside world. As an addict, I can say that we think we are dependent on it and need that fix. We know, in the back of our mind, that we don't actually need the drug to have a better quality of life. The people who do need and deserve to have a drug to quell physical pain, do so because they just want to feel somewhat human again. It helps them manage through the day or week; to feel any kind of normalcy in their waking life. I know my father is one of them. His inability to get treatment during this ‘epidemic’ is limiting his ability to get out of bed in the morning and do simple things like, going to the store, or putting on shoes, or getting a shower. It’s unfortunate that we deprive everyone in need, because of the few.
Perspective from a Former Pain Management Clinic Staff Member
I talked with a health practitioner who requested that I not use her name. She worked as the new patient coordinator at a pain management clinic in central Texas. She shared that in Texas, they have federal and state guidelines to follow when prescribing medications. The clinic she worked at had many people prescribed opioids for legitimate pain issues for years. But then it had to reduce those prescriptions by half when opioid restrictions were enacted.
According to her, “The limitations on medication applied to just about everyone, with the exception of some cancer patients. But even then, it was difficult to get opioids approved for those who really needed them. We had a sweet lady who battled cancer for 20 years. Previously, her oncology doctors prescribed her medications. However, due to federal regulations, they had to refer her to a pain management practice, which is how she came to us. Her insurance company gave us a hard time about prescribing the medication she needed to keep her comfortable. It was a ton of paperwork, and the insurance companies played games with us. If it wasn’t the restrictive government regulations causing problems, it was the insurance companies.”
In a phone interview, I asked her a couple of questions to draw out more information about her insight and experience.
Question 1:
Rachel: What’s the underlying, root problem?
Her response: It’s a combination of the government regulations, insurance protocols, and chain pharmacies that are the biggest problems for doctors. Hardly any doctors will give hydrocodone without a lot of proof that a patient needs it. The bad thing is that patients build up a tolerance to it.
Insurance companies want people to go through physical therapy, but that sometimes makes things worse and intensifies their pain problems. We had patients who could hardly move after PT sessions, but they were required to do it anyway.
Our physician was constantly worried about prescribing opioids—even for those who genuinely could benefit from them— for fear that would lead to an audit and possibly a fine.
I don’t know that there is an answer in sight for the problem; there are people out there who need opioid medications.
Sadly, the way Medicare is handled is a real issue, too. When patients fall in the “donut hole,” and they are on a fixed income, some may have to choose between whether they will pay for their pain medications or buy groceries.
Question 2:
Rachel: Based on what you’ve seen, what needs to be done to make this situation better?
Her response: For one thing, I believe doctors should have the authority to make the decisions for their patients without interference from the insurance companies. The three doctors I worked with at the clinic had their patients’ well-being at heart. They know which patients will have a better quality of life with certain treatments over others. Unfortunately, physicians also have to answer to the insurance companies. Physical therapy was a required insurance protocol. They want to rule out that PT won’t help. The next step is steroid injections, then nerve blocks (both of which only last a few days), and then RFA (radio frequency ablation). If none of those work, then either surgery or pain meds are next. Yet, you have to jump through hoops to treat them with those things.
Unfortunately, there are bad doctors out there, who have ruined it for the good ones. I know of two doctors arrested for running pill mills, and both were drug addicts. They lost their medical licenses. I don’t think they were planning to do anything illegal, but they got sucked into it. Doctors like that are a real part of the problem, one that no one really talks about.
The most distressing and disheartening impact is that patients who really, really need the medications are unable to get them.
Pain Patients – “Collateral Damage” of the Opioid Crisis
My dad shared that the first time a doctor gave him oxycodone was in 1999, “It was something that allowed me to function and work. I finally felt useful. Without the pain holding me back, I enjoyed having a job again.”
But then opioids became Public Enemy #1. And, after 20 years of taking the only medication that allowed my father to be an active participant in life, he was told by his doctor that he could no longer have it.
Why? The Pennsylvania District Attorney sent Dad’s doctor a letter threatening to take away his medical license if he didn’t cut back on prescribing opioids.
“What’s happened with the opioid battle is not just cutting back patients’ meds. They don’t want to give you anything at all. Nothing. They cut back the prescriptions and dosages quickly—and then they drop you like a hot potato,” said my father. “My doctor, without any advance notice, told me I needed to go to a treatment center and see an addiction specialist because going off my pain meds would cause withdrawal symptoms.”
Now, not only is my dad in constant pain, but he’s also worried about whether another doctor will take him as a patient since he was sent to an addiction treatment center—even though it was to avoid getting sick from going off of the medicine he legitimately needed for quality of life.
How Did We Get Here and Where Are We Headed?
Dad is one of many people in the U.S. who deal with pain that impacts their lives day-in and day-out. A National Health Interview Survey in 2019 reported that 20.4 percent of adult respondents in the United States said they have chronic pain. Moreover, 7.4 percent of those survey participants said that they have chronic pain that often interferes with life or work activities.
I have to wonder how many Americans with debilitating pain are being denied quality of life.
I’m sure there are a multitude of reasons why we are where we are, but from what I gather, much of it began when the CDC (Centers for Disease Control and Prevention) issued a “Guideline for Prescribing Opioids for Chronic Pain” in 2016 to recommend that primary care practitioners do not prescribe opioid dosages above 50 morphine milligram (MME) equivalents or less for new patients. It also advised physicians to conduct risk/benefit reviews for any patients on existing prescriptions for doses above 90 MME. (By the way, 50 MME per day equates to 50 mg of hydrocodone, 33 mg of oxycodone, or 12 mg of methadone. 90 MME per day equates to 90 mg of hydrocodone, 60 mg of oxycodone, or 20 mg of methadone).
The introductory language of the Guideline explicitly states, “The recommendations in the guideline are voluntary, rather than prescriptive standards. They are based on emerging evidence, including observational studies or randomized clinical trials with notable limitations. Clinicians should consider the circumstances and unique needs of each patient when providing care.”
However, many primary care physicians, insurance companies, hospitals, and legislators appear to have interpreted them as mandates for the limits to be followed when prescribing opioids for anyone, including patients who rely on them for pain management and haven’t abused their use. In fact, in two years after the CDC released their Guideline, over half of the states in the U.S. enacted legislation to implement opioid prescription limits and apply them across the board. Their laws were applied to not only the CDC’s intended audience, primary care physicians, but also dentists, physician assistants, nurse practitioners, and…wait for it…pain specialists! Compounding the issue is that some national chain pharmacies began black-listing medical professionals who are high prescribers of opioids.
In 2018, the American Medical Association House of Delegates issued a resolution (Resolution 235-I-18) which addresses the fact that the CDC’s Guideline is being applied to all patients equally, without regard for their individual circumstances. It calls out legislators for initiating policies that are too restrictive, “While it is common for state opioid prescribing restriction policies to allow for exceptions for patients with cancer, in hospice or who require palliative care, to name a few, exceptions are highly variable regarding post-operative surgical care, chronic pain, cancer remission-related pain, sickle cell or other conditions for which a patient might require a prescription for a greater dosage than a state law might allow.”
The AMA expressed its opposition to the hard limits, explaining that patients who fall into the state’s exact exception categories and are denied the opioids they need to manage pain are put in potential danger as a result.
Even the CDC’s Guideline acknowledges that, “There are clinical, psychological, and social consequences associated with chronic pain including limitations in complex activities, lost work productivity, reduced quality of life, and stigma, emphasizing the importance of appropriate and compassionate patient care. Patients should receive appropriate pain treatment based on a careful consideration of the benefits and risks of treatment options.”
Also, the FDA (Federal Drug Administration) issued a safety announcement in April 2019 that sudden discontinuation or rapid decrease of opioid pain medications can cause “serious withdrawal symptoms, uncontrolled pain, psychological distress, and suicide.”
There you have it. Chronic pain poses a danger to people. Sadly, patients with that intensity and duration of pain are not getting the medication they need to function and live comfortably. They’re caught in the crossfire in the war against opioids.
Final Food for Thought
I realize that writing about this might not change anything, but I felt compelled to talk about it. If it helps even one person see the opioid crisis through a different lens, I believe my effort here has been worthwhile. I’ll let you draw your own conclusions. If you agree, I invite you to share this post to help spread the word on this very important topic.
~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~
Resource:
This Tedx Talk, from Dr. Stefan Kertesz, offers insightful information about the negative impact on patients who rely on the drugs to combat ongoing pain. Sadly, the government, insurance companies, and others parse and manipulate data to serve their purposes.
Sources and References:
CDC – Calculating Daily Dose of Opioids
CDC - Chronic Pain and High-impact Chronic Pain Among U.S. Adults
CDC Guidelines for Prescribing Opioids for Chronic Pain
AMA
Stat News
FDA

Wonderful and thorough piece. I can truly relate. I had my meds taken away (cold turkey, no slow down) so I had a bad reaction and have had a very low quality of life for the past few years. I don't eat very often or shower. I mostly lay in bed. Earlier this month was my 18th year anniversary of getting RSD/CRPS. It's commonly called the Suicide Disease. I have come very close a few times to taking my life over the past 18 years to giving up. When they took my meds was the closest. It was awful. I have a barely helpful pain med now. I was on a very low dose of methadone and stable for around 12 years. There was zero reason to disrupt me. And now they have no motivation to take me back because it is too dangerous. Too dangerous to give me a life? I said if it takes 5 or 10 years off my life, who cares? It allows me to have some functionality and not be so miserable. I've told them a would sign a release and so would my family that no lawsuit would be filed if something happened to me. I've written my fed & state lawmakers. It's like no one cares. Oh, but they care about the addicts. Why do their lives matter more than mine? They asked for their problems, I didn't. They could stop what they are doing. I have no control over it. And I completely understand drug addiction. I was married to an addict for many, many years. I lost a bro in law to addiction and my uncle was a drug addict (he died in a car accident). I'm not saying I'm better than addicts, I'm saying they have more control. And it sure seems like the government, doctors, etc are all putting their lives ahead of mine. Anyway, I didn't mean to get so carried away. This is a passionate topic for me. Also, people think we take pain meds and are drug out feeling good. These meds take the edge off at best. They don't make us feel high or good. At least they never did for me. I should be able to decide with my doctor without him worrying about the government coming after him. There is a long list of rules you have to follow. If you are good with those with your doctor and he is doing what he is suppose to do with the already established rules then there shouldn't be a problem. The "opioid epidemic" has been going on for a very long time just with different drugs. Addicts will take whatever they can get their hands on and they will do whatever it takes to get their hands on what they want. Punishing people who already have miserable lives isn't going to change that. Good luck and take care to you, your brother, and your poor dad. Sarah
Hi Rachel! I came across this piece you wrote on your strellasocialmedia.com. I just wanted to say thank you on behalf of intractable/chronic pain patients everywhere. I’m so sorry about your father having to live with so much pain. I’m also very glad your brother is doing well.
This side of the opioid crisis almost never gets told. A huge misinformation campaign by the CDC, other agencies and the complicit media has made it difficult. Media looks for sensationalism and the mega billion dollar lawsuits against big pharma are driving the news cycles as relating to the opioid crisis.
The litigation firm, Motley Rice, who won the settlements from big tobacco years ago, is the same law firm currently litigating against big pharma and they unfortunately, have a huge influence over MSM. What we have seen by MSM over the past few years, instilling addiction phobia, is nothing more than attempt to sway the jury pool for these lawsuits, at least in my and many other’s opinions.
These multi million number of diverted pills claimed by the DEA, that they let happen, is no doubt, accurate. But, these are not from pain patients as we were led to believe. Chronic pain patients need their medicine to have any decent quality of life. Now, the pharmacy distributors, rogue pharmacies, pill mills, rogue Drs and others in the medical field - that’s where the problem was. This recent article drop from the DEA about diversion, tells a lot of the story.
Also, this article that was dropped yesterday, tells the story about the lies and deceit by the CDC, and how they duped our country into demonizing Rx pain medicine. The real scourge is illicit fentanyl and it’s hundreds of analogs, along with heroin, meth and a resurging cocaine market are what’s driving the ODs. A few years back, yes, Rx pain medicine was causing unnecessary ODs, together with multi substances abuse including alcohol. It’s known as polypharmacy. I will post a PDF document summary for you and here’s the link for your reference. One of the authors is a former DEA agent.
very good article..helps explains a few things..
Thank you for telling the other side of the issue of pain meds. My husband hashad 9 back & neck surgeries and they have cut him back horribly! In fact he gets yet ANOTHER cut back in April. He already has beencut back to half what he had before and they are still lowering it. He can only sit in his chair miserable all day. I myself have bulging discs in neck and low back and I cant take nsids. I am on minimal meds & can hardly function & Im only 46. No quality of life what so ever. I have known several people who switched to heroin because doctors took away pain meds they legitimately needed. So sad. Doesnt the cdc, fda & dea realize that they are fueling the HEROIN epidemic by taking pain meds legitimately needed away from people? Something REALLY needs to be done!
This is a short "well done". This narrative is grounded on personally observed experience as well as research on the facts of chronic pain versus addiction.
I'm a technically trained healthcare writer and patient advocate for people in pain. I've created and moderated social media patient support groups for almost 25 years. I write extensively on the misdirection of US regulatory policy for prescription opioids and doctors who employ them on behalf of their patients. If you ever need something researched, feel free to call on me. I'm easy to find.
Thank you for bringing attention to the horrific collateral damage that has been done to chronic pain patients. We never ever were the issue that spiked the overdose crisis but the media sure loves to paint all of us with this broad brush. Addicts will just move onto a new drug of choice when their other supply dries up. Chronic pain patients don’t have that luxury. Sadly those that are making policy against us will never have to worry should they get hurt or injured. They will never be told no opiates don’t work instead they will be asked what drug do you prefer and how many pills would you like. It’s hard not to feel hopeless when no one is hearing our cries for help.
Thank you for speaking up for those of us who find it hard to express our frustration that no one is listening unless you are experiencing chronic pain oneself. Its hard to put into words what I've been going through over the past few years. Ice ran through my veins when a pain managment doctor told me she doesn't want to treat me because my "number" is to high. She says "they" would come for her license. I have so much to say but I'm in too much pain to sit and type. I am afraid that I will not have my pain treated in my life time. I'm sorry if I'm not articulate enough. I just hope someone is listening.